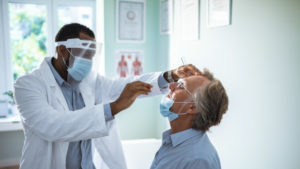
The market for COVID-19 diagnostic kits is much broader than just the health sector, as miners and other industries begin to compete for tests with governments.
But where diagnostic tests normally require at minimum several months of patient data behind them, the current emergency means kits are needed now, without the usual supporting data.
It means, according to experts in diagnostics and biotech investment, there will be some tests that can’t be 100 per cent positive that a negative result is correct.
That is not deterring big business or governments.
Already governments from Italy, Germany and the UK, to New York are looking at COVID19 or immunity “passports” to allow people with coronavirus antibodies — proteins created by the immune system against a pathogen — to move freely again and start to reopen economies.
Companies too want methods to protect the employees they have left and find ways to bring people who may have immunity against COVID19 back to work.
Diagnostics is big business
Australia’s medical regulator the Therapeutic Goods Administration (TGA) has approved 17 tests for use in Australia that have been sponsored by 20 companies (some companies are importing the same test).
Federal and state governments are desperate for diagnostic kits.
But industry want their own as well.
“As soon as we said we had a test we were absolutely overwhelmed,” said Cellmid (ASX:CDY) chief Maria Halasz, with emails from members of the public wanting to be tested, government agencies, and companies.
Cellmid has been in touch with “literally all of the mining companies” which want to have the tools on hand to find out if remote mining sites become loci for the virus and be able to bring back people who have had it.
Halasz says aged care homes are also keen to stockpile their own tests.
Cellmid is importing a kit from China that tests for antibodies which show whether a person has had COVID-19 in the past.
The science is still out however on whether COVID-19 antibodies do confer immunity against the disease, and if so how much.
In the medical sector, demand is for diagnostics that show whether a person has the virus, now; these test for the viral RNA, an antigen or foreign substance that causes an immune response in the body.
The demand here is from pathology and microbiology labs, says Genetic Signatures (ASX:GSS) chief John Melki, like Sonic Healthcare (ASX:SHL) and Healius (ASX:HLS).
Melki says there has been interest from the mining and food sectors for the test Genetic Signatures designed using its own diagnostic technology, but they are prioritising pathology labs.
Equal interest has been from ASX companies which has landed at least one in hot water: TBG Diagnostics (ASX:TDL) said its Chinese subsidiary had European regulatory approval for a test, but told the market four days after it found out.
Diagnostics to doggie suppliers
Genetic Signatures made its own test using a technology it has been developing for 12 years, and if it gets TGA approval it will join AusDiagnostics as the only other Australian-made test on the list.
Of the 17 manufacturers with COVID-19 tests listed on the Australian Register of Therapeutic Goods (ARTG), eight are Chinese and six are from the US.
Nine of the tests are point-of-care antibody tests that can be administered on the spot by a medical professional.
The remainder are antigen lab tests.
Sponsoring them are companies like Cellmid, which specialises in hair regrowth treatments and an early stage anti-inflammatory treatment, major healthcare companies like Roche and Hologic, and specialised diagnostics companies like Integrated Sciences.
But the list also includes a range of unlikely importers that don’t have biotech or lab experience on their resumes.
There’s a Chinese-Australian medical tourism company called Medicision, a company that sells explosive and chemical detection kits called APAC Security, and a pet supplies company called Envon.
So what are these tests?
There are two main types of tests.
The antigen test is best used for frontline diagnostics, where medical professionals need to know if a person has COVID-19, while the antibody test can be used to find out whether people who are asymptomatic have had it.
The first looks for viral RNA using polymerase chain reaction (PCR), a method that has been standard practice in labs for 30 years to multiply a very small sample. It can detect the virus from as little as a single particle from a mouth, nose or throat swab.
Countries relied on these at the start of the pandemic as they are fast to develop and give very accurate positive results.
The downside is they take anywhere between hours and days to return a result — the fastest machine takes two hours — and are expensive, because they need to go to a lab for analysis.
And if a patient has a low viral load — they don’t have much of the virus — there is a risk that the part of the sample that’s tested doesn’t include a virus particle, meaning they can return false negatives.
The second test looks for antibodies, which are created seven to 11 days after a person catches a virus and can deliver results in as little as a couple of minutes. This is a blood or ‘serology’ test that functions like a pregnancy test, with one line for negative and two for positive.
They can be a powerful tool to check if vaccines are working, wrote University of Reading associate professor Alexander Edwards in The Conversation, but they take time to be tested with many different samples to make sure they’re fully reliable, accurate, and to know how soon after infection they work.
“Rapid tests are quick to manufacture and easy to use but have to be carefully designed and validated, which is why they are not approved for use and we haven’t seen widespread official use yet,” he wrote.
“Quality control and validation adds significant cost to these tests.”
The Royal College of Pathologists of Australasia last week came out forcefully against antibody tests, saying they “have no role to play in the acute diagnosis of COVID-19 virus infection” and “will miss patients in the early stages of disease when they are infectious to other people”.
It’s a claim Cellmid’s Halasz says is self-serving, as rapid antibody tests don’t require a pathology lab.
Will they work?
The question is whether tests that don’t have the usual level of patient data and testing behind them will work to the level required to be safe.
The urgent need for diagnostic tests led to fast-tracked approvals for 17 tests, on condition the sponsor companies report safety and efficacy data within 12 months. It has also contracted the Doherty Institute, which mapped the COVID-19 genome, to assess, trial, and validate unapproved diagnostic test kits.
COVID-19 tests are also allowed to be sold directly to registered pathology labs without being put on the Australian Register of Therapeutic Goods (ARTG), under an emergency exemption.
Morgans analyst Derek Jellinek says sensitivity (the ability of a test to correctly identify those with the disease) and specificity (the ability of the test to correctly identify those without the disease) is critical for these tests.
Cellmid’s test has clinical data from 596 clinical samples showing specificity of 99.57 per cent and a sensitivity of 86.43 per cent on day three and 95 per cent on day five of infection.
Melbourne-based MD Solutions, which had its test approved two weeks ago, says after five days of infection its test has a 96.9 per cent sensitivity rate and 99.4 per cent specificity rate.
You might be interested in